[embedyt] http://www.youtube.com/embed?layout=gallery&listType=playlist&list=UUmJowplQ1zMtfq5hdTVQqrQ[/embedyt]
Inversion Tables for Lumbar Discogenic Pain
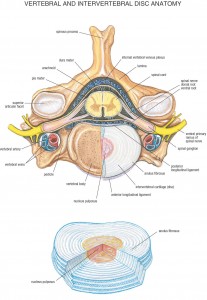
Discogenic pain presents as localized pain at the spine, most often the lumbar spine that worsens with lifting, coughing, sneezing, or straining during a bowel movement. Discogenic pathologies include bulging or herniated intervertebral discs, degeneration of a disc, dehydration of the disc nucleus, or tears in the fibrous capsule (annulus) of the disc. A malformed or degenerated disc can result in the boney vertebrae moving closer together causing peripheral nerve impingement at the neural foramina.
Inversion tables use gravity and your body weight to traction the spine. As the spine stretches, it creates a negative pressure within the intervertebral discs. The negative pressure, in conjunction with osmosis, pulls water into the gelatinous center of the disc called the nucleus pulposus. Stretching and hydration thicken the discs and lengthens the spine. As the discs thicken the separate the vertebra and increase the free space around the nerves as they leave the spine- the result is a healthier and happier you.
What are the contraindications for inversion tables?
Inversion tables take a little coordination and possibly even some assistance. Most inversion tables work by setting the maximum decline angle, locking your ankles into the suspension, then leaning back and slowly tilting backward until your head is below your ankles. This seemingly simple process can be problematic if you have the following issues:
- Retinal detachment
- Stroke
- Recent head injury
- Spinal injury
- Bone weakness
- Lumbar fusions, either surgical or from bone remodeling
- Severe osteoarthritis of the facet joints of the spine
- Tears in the vertebral discs
- Vestibular problems resulting in dizziness and nausea
Geriatric patients or patients with disabilities should not use inversion tables without assistance and clearance from their primary care physician.
When will I feel better?
When patients first begin stretching their spine, it can result in increased discomfort for 1-2 weeks. The reason for this is that the musculature of the spine has contracted to protect and stabilize the injured area. The problem with this is that the increased muscle contraction also creates more pressure on the discs, flattening them out and reducing their ability to rehydrate fully. Increased disc compression with dehydration equals prema ture disc degeneration.
Relief can be immediate but short-lasting. Long-term results will take 4-8 weeks of tractioning five times per week. After the discogenic pain has resolved, a maintenance tractioning program of 3-4 times per week is recommended.
When should I do traction and for how long?
Traction should be performed just before bedtime for 5-10 minutes. Tractioning just before bedtime allows you to lay flat after stretching the discs, so gravity doesn’t recompress the spine before they get a chance to rehydrate.
Stop traction if your pain significantly increases.
Even though your might get slightly worse before getting better, a dramatic worsening in your condition the following traction may indicate that there is a more significant spinal pathology occurring and further diagnosis is required.
Treatment of Plantar Fasciitis Foot Pain

Foot pain is a very common ailment that can range from mild discomfort too a debilitating condition that limits ones quality of life. Plantar fasciitis is a frequently diagnosed condition characterized by chronic heel pain and pain along the sole of the foot. Although there are several conditions that exhibit this pattern, plantar fasciitis displays a symptom called “poststatic dyskinesia,” which is pain with increased intensity when rising from a resting position. People with plantar fasciitis frequently have severe foot pain when they first get out of bed in the morning, but the pain diminishes with activity and later returns as the day wears on.
Multiple Causes of Foot Pain
Plantar fasciitis can have several different causes but is usually a result of repetitive stress injuries to the feet. This condition is commonly seen in patients who stand on hard flat surfaces for prolonged periods of time. Runners and joggers that train on pavement are prone to this condition. Plantar fasciitis can also occur for no known cause or as part of the aging process. A professional medical diagnosis should be made to determine the appropriate treatment approach. In addition to plantar fasciitis, there are several other possibilities that can cause foot pain and require a differential diagnosis, some of these include peroneal tendonitis, gastro-soleus complex, plantar calcaneal bursitis, metatarsalgia, heel fat pad syndrome, and several others.

Scar Tissue and “Bone Spur” Formation
Scar tissue may form at the heel of the foot as a result of chronic irritation and inflammation of the plantar fascia. If the inflammation, scarring, and irritation become chronic they can resulting calcification of the fascia at its attachment point on the calcaneal (heel) bone. This calcified fascia appears on a foot x-ray as an hook shaped bone spur on the sole of the foot at the heel. When fasciitis goes untreated and becomes chronic to the point of bone spur formation, non-invasive techniques may not be effective and surgery is often required.
Treatment Approaches Provided by Medical Practitioners
Practitioners such as chiropractors, physical therapists, acupuncturists, and massage therapists can provide a variety of effective modalities for the treatment of plantar fasciitis. Techniques such as micro current, ultrasound, interferential, acupuncture, transdermal medications, and manual therapies can provide effective and permanent pain relief. Physicians can inject a steroid into fascia attachment at the heel to reduce local inflammation.

Foot Orthotics and Shoe Inserts
The opinion of using inserts and orthotics is more a matter of philosophy than medical science. Some practitioners believe that providing arch support in the form of orthotics will take pressure off the plantar fascia and allow it to heal. Others believe that the arch naturally falls with normal wear and aging of the feet. As the arch begins to break down and drop, there is increased tension on the fascia as the foot elongates, which causes inflammation and pain in the sole of the foot. In this case, practitioners encourage stretching the fascia to allow for the new foot position so the fascia can heal on its own. Hard orthotic inserts are believed by some to only further weaken the arch and prolong irritation of the plantar fascia.

Self-Help Remedies
The #1 most common self-help treatment for plantar fasciitis is golf ball massage. Yep, a plain old golf ball. Placing a golf ball on the ground and then rolling it under the sole of your foot will stretch the fascia and improve circulation. The golf ball is just the right size and shape to effectively massage the sole of the foot.
Heel lift inserts, or just wearing shoes with ½ inch to 1 inch heels, can be beneficial and provide relief for some people when tight calf muscles and/or Achilles tendinitis may be contributing to the foot pain.
Calf stretches with full extension of the toes (pulling the toes up) is a good stretch for the plantar fascia. There are foot supports that can be worn at night that keep the ankle flexed and toes extended to stretch the fascia while you sleep.
Hot water foot soaks. Although ice may feel good and temporarily numb the area, ice causes constriction of blood vessels and slower healing times. Unless there are acute signs of redness, swelling, heat, and pain, or you just need some immediate pain relief, it is best to avoid ice and stick with heat. When in doubt as to use heat or ice, do what provides the most relief.
Tips for reducing joint pain and increasing movement
- Start moving. Joints are designed to move and reducing movement also reduces synovial fluid lubrication and blood circulation within joints.
- Perform static flexion of joints for a minimum of 2-3 minutes prior to exercise or prolonged activity. Full flexion of a joint decreases joint pressure and distributes lubricants across the joint space.
- Move joints through a full range of motion. Limiting joint movement causes uneven wear on joints.
- Joints that “give out” are typically the result of issues with the muscles and ligaments that cross the joints. Maintaining good muscle tone is essential for joint stability.
- Edema and swelling in and around joints (joint effusion) can contribute to joint pain. Wearing thin, flexible compression sleeves over joints (i.e. ankles, wrists, knees, and elbows) combined with the “pumping” action of joint movement can reduce or prevent joint swelling.
Dietary Recommendations
- Glucosamine sulfate, a supplement found in the exoskeletons of crustaceans, has been shown to ease joint pain and stiffness in joints if taken during early onset. Dose: 1,500 mg (1.5 gm) per day.
- Omega-3 fatty acids have been shown to have anti-inflammatory and pro-resolution properties. These fatty acids stimulate the clearance of inflammatory debris, promote mucosal antimicrobial defense, protect organs from collateral damage, and enable inflamed tissues to return to homeostasis. Dose: 1,240 mg (1.24 gm) per day.
- Herbs such as turmeric, ginger, and boswellia may also be beneficial as natural anti-inflammatories. Bromelain, a pineapple enzyme, has also been used as an anti-inflammatory when taken in doses of 200-400 mg per day on an empty stomach.
- S-adenosylmethionine (SAMe) is found naturally in the body. SAMe supplementation has been found to be as effective as and safer than non-steroidal anti-inflammatory drugs (NSAIDs) but has a slower onset time. Dose: 400 mg 3-4 times per day for 1-12 weeks.
Supplements that may ease symptoms of migraine headaches
- Feverfew Leaf
50 mg daily or 125mg dried feverfew leaf from Tanacetum parthenium
High in Sesquiterpene Lactones (STL) of which must contain at least 0.2% parthenolide content.
- Ginger
500-600 mg powder—every 4 hours for 4 days
Pro-inflammatory mediator; inhibits platelet aggregation.
- Ginko Biloba Extract
120-240 mg per day
Platelet-activating Factor (PAF) antagonist.
- Magnesium
200-360 mg per day
Inhibits vasospasm and platelet aggregation.
- Riboflavin
400 mg per day with breakfast for at least 90 days
Involved in the electron-transport chain.
- L-Tryptophan
500 mg per day for 90 days, every 6 years
Precursor to scrotonin production.
- Fish Oil (omega 3 fatty acids)
Inhibits platelet aggregation.
- Maintain blood sugar levels—eat small meals throughout the day.
AVOID:
–Tyramine (a vasoactive amine) in foods such as aged cheese, yogurt, beer, wine, liver, and yeast.
-Foods that may be allergens.
Nutritional Recommendations for High Cholesterol (Hypercholesterolemia)
- Chromium picolinate 200 mcg with Niacin 50-100 mg (flushing type) have a
 synergistic effect at lowering cholesterol levels and enable the dose of niacin to be reduced without reducing its effects.
synergistic effect at lowering cholesterol levels and enable the dose of niacin to be reduced without reducing its effects. - Vitamin E 800 IU daily. Vitamin E causes an increase in HDL. May be taken with Selenium 200 mcg, which has a synergistic effect with vitamin E.
- L-Carnitine, Taurine, and 50-200 mg per day of Co-Q10 may improve the ratio of high density lipoproteins (HDL) and low density lipoproteins (LDL).